Infectious disease can afflict a population in complex ways. Understanding the varying risks is an equally complex challenge.
The Centers for Disease Control and Prevention (CDC) offers a general metric for assessing the risk of natural disasters in a region in terms of Social Vulnerability Index (SVI), which includes socioeconomic and cultural factors that impact how a region can adapt to a disaster. Researchers at Washington University in St. Louis wanted to take a more specific approach for assessing a state’s risk for influenza-like illness.
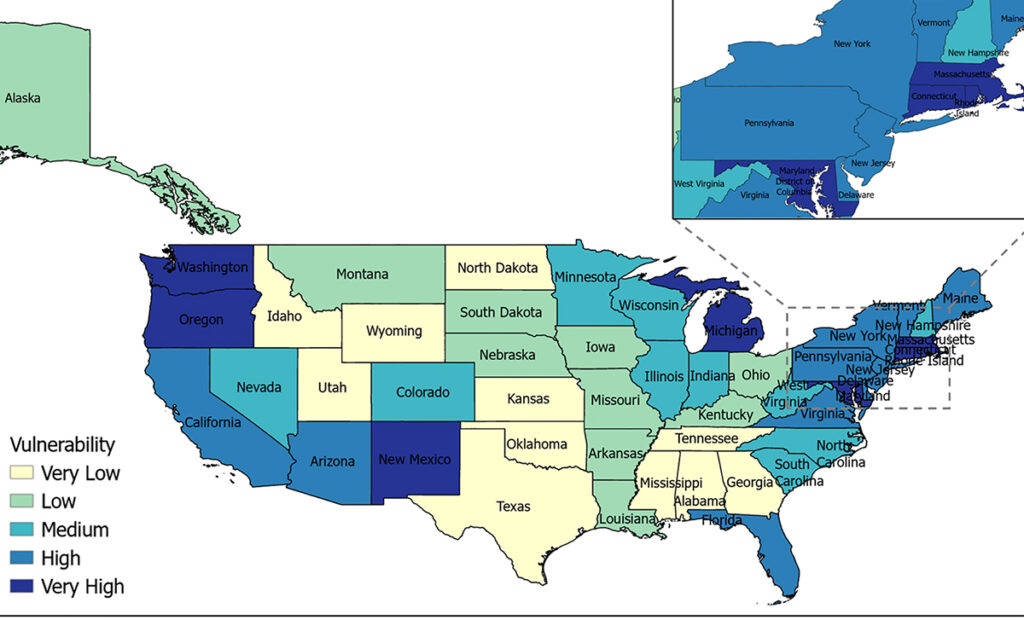
Their work, now published in the journal PLOS Computational Biology, provides a state-level vulnerability map revealing significant regional disparities between states at higher risk for infection.
“This approach considers the relative importance of the many socioeconomic and health factors within a defined area,” said Rajan Chakrabarty, the Harold D. Jolley Professor of Engineering in energy, environmental and chemical engineering at the McKelvey School of Engineering at WashU.
He added that the index can provide vulnerability “hotspots” in the U.S. so that policymakers can develop better targeted strategies to prevent the spread of flu.
Unlike previous models that mostly rely on health data for determining a region’s disease risk, Chakrabarty’s team used machine learning algorithms that can crunch census data and determine the non-linear relationships between socioeconomic factors, health indicators and vulnerability to flu.
All told, the new index integrates 39 socioeconomic and health indicators from census data including factors like migration patterns, insurance coverage and proportions of female and elderly populations.
“Vulnerability does not come from a single factor, but is shaped by urbanization, demographics, healthcare access and economic disparities,” Chakrabarty said.
Each state has its own unique “fingerprint” of risk factors, neatly mapped out in the research.
Policymakers in some places may need to better understand the combined effect of different socioeconomic factors on disease spread, like in more dense metros with a high number of foreign-born populations. People in other places may need to connect neglected rural population to insurance and health care or provide poverty relief programs that link vulnerable groups to healthcare access. All states will likely need to do “all the above” in some form, Chakrabarty said, but they will benefit from putting extra resources where targeted interventions might make the biggest difference.
For example, the District of Columbia, is the most “at risk” region in part because it is characterized by high population density and mobility (which allows easy spread of viruses) and increased risks due to a sizable uninsured foreign-born population and longer commute times.
In contrast, states with large rural regions, such as New Mexico and Arizona, also exhibit heightened flu vulnerability. But in these states the vulnerability is due to different factors, like the higher numbers of aging, female and Hispanic people — a population more at risk for flu complications.
Michigan is another high-risk state because of its mix of urban and rural regions. Michigan faces dual challenges — high transmission risks in cities and economic hardships in rural areas — noted Shrabani Sailaja Tripathy, postdoctoral associate in Chakrabarty’s lab and lead author of the research.
Every state has a complicated picture, but policymakers now have a new tool that they can apply when they consider vulnerability to any infectious disease, Tripathy said.
“This can help strengthen our epidemic preparedness and response,” Chakrabarty said.
Tripathy SS, Puthussery JV, Kapoor TS, Cirrito JR, Chakrabarty RK (2026). Spatial variation in socio-economic vulnerability to Influenza-like Infection for the US population. PLOS Computational Biology 22(1): e1013839. DOI: https://doi.org/10.1371/journal.pcbi.1013839
This work was supported, in whole or in part, by Flu Lab.