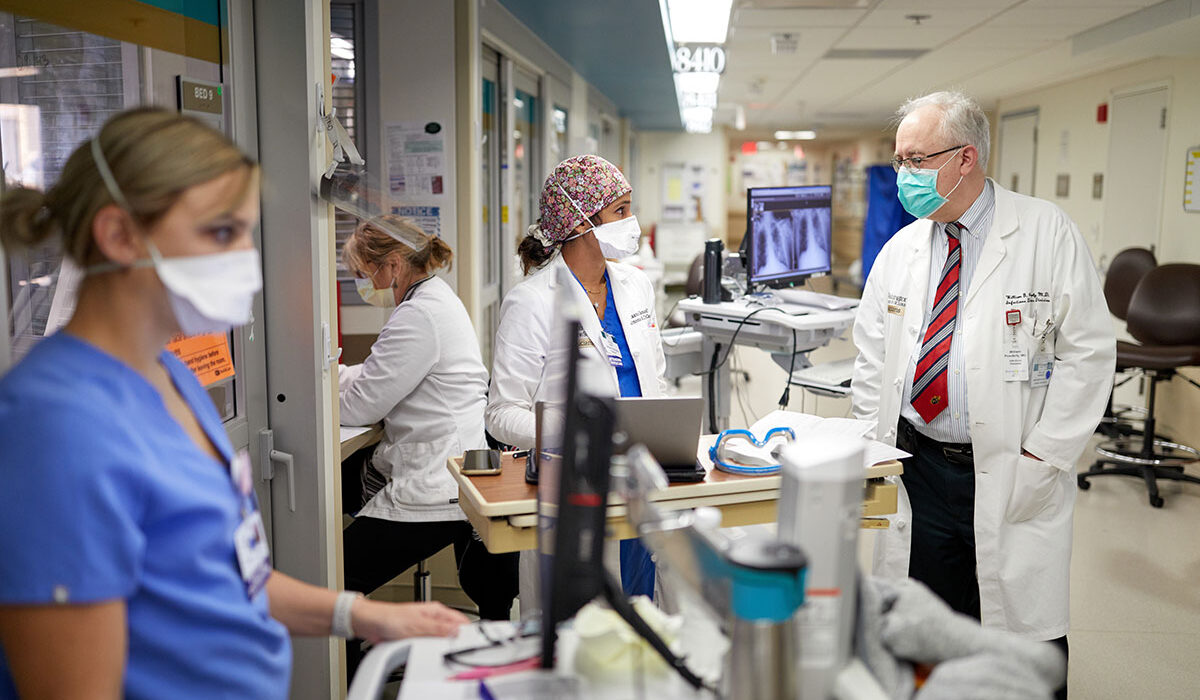
Two drugs commonly used to treat inflammatory diseases such as rheumatoid arthritis and psoriasis did not shorten recovery time for patients hospitalized with severe COVID-19 but did reduce the likelihood of death when compared with standard care alone, according to a national study led by Washington University School of Medicine in St. Louis.
The study was funded by the Biomedical Advanced Research and Development Authority (BARDA) of the Administration for Strategic Preparedness and Response within the U.S. Department of Health and Human Services (HHS). The study was coordinated by the National Center for Advancing Translational Sciences (NCATS) of the National Institutes of Health (NIH), also part of HHS.
The study is published in JAMA.
In April 2020, the NIH launched a public-private partnership called Accelerating COVID-19 Therapeutic Interventions and Vaccines (ACTIV), with the ultimate goal of speeding the development of the most promising COVID-19 treatments and vaccines.
As part of this partnership, a clinical trial called ACTIV-1 Immune Modulator (IM) was developed to compare multiple drugs at once. The researchers evaluated three anti-inflammatory drugs — infliximab, abatacept or cenicriviroc — added to standard care versus standard of care alone, in participants hospitalized with COVID-19. Standard care for such patients includes remdesivir, an antiviral drug, and dexamethasone, a corticosteroid. The study included 1,971 patients treated at 95 hospitals in the U.S. and Latin America. Many of these sites were supported by the Clinical and Translational Science Awards Program, funded by NCATS.
Even in the earliest days of the COVID-19 pandemic, it was evident that the body’s aberrant and dysregulated immune response to SARS-CoV-2, the virus that causes COVID-19, is often responsible for pneumonia, respiratory failure and other severe consequences of the disease.
“One of the fundamental questions of early COVID-19 research was whether we could dampen the inflammatory process using existing anti-inflammatory drugs,” said William G. Powderly, MD, the J. William Campbell Professor of Medicine & co-director of the Division of Infectious Diseases at Washington University School of Medicine in St. Louis. Powderly served as the national principal investigator leading the ACTIV-1 trial. “Our data suggest that two of the drugs we studied can be given to reduce mortality in severely ill patients. We hope this study will be helpful in revising guidelines for best practices in treating patients hospitalized with COVID-19.”
When used in conjunction with standard of care, these immune modulators did not yield a statistically significant difference in recovery time compared with no use of such medications. However, Powderly said two of the three drug treatments still have clinical importance, especially in terms of one of the study’s key secondary endpoints: mortality. Fewer patients died when treated with standard care plus either infliximab or abatacept, compared with patients who received standard care plus a placebo. Treatment with the third drug, cenicriviroc, was stopped early because the data showed no benefit.
Sold under the trade name Orencia, abatacept is used to treat joint swelling, pain and fatigue associated with rheumatoid arthritis. It is administered via infusion and works by reducing T cell responses. Infliximab, known by the trade name Remicade, is used to treat adults with rheumatoid arthritis in combination with methotrexate, and adults with chronic severe plaque psoriasis, among other conditions. Abatacept and infliximab were administered via a single infusion in the ACTIV-1 trial.
For COVID-19 patients treated with abatacept, 56 out of 509 patients had died by day 28 (11% mortality). In the placebo group, 77 out of 510 patients had died over the same time frame (15.1% mortality). This 4.1% difference represents 21 fewer deaths among those who received abatacept.
For patients treated with infliximab, 52 out of 517 patients had died by day 28 (10.1% mortality). In the placebo group, 75 out of 516 patients had died by day 28 (14.5% mortality). This 4.4% difference represents 23 fewer deaths among those who received infliximab.
Although this study’s immune modulators, when used in conjunction with standard of care, did not yield a statistically significant difference in recovery time, the mortality numbers determined by this study are still considered clinically important, according to Powderly. He said this type of study is crucial for patients hospitalized with COVID-19, as it means that potential options for treatment continually are expanding.
“We’ve now shown that there are multiple potential options available for COVID treatment,” Powderly added. “But ideally, we as doctors don’t want to have to treat COVID pneumonia. We much prefer to prevent it, and vaccines are still the best way to prevent severe COVID-19.”
O’Halloran JA, et al. Abatacept, cenicriviroc, or infliximab for treatment of adults hospitalized with COVID-19 pneumonia: a randomized clinical trial. JAMA. July 10, 2023.
This work was funded by the U.S. Department of Health and Human Services, Administration for Strategic Preparedness and Response, Biomedical Advanced Research and Development Authority, under contract number HHSO100201400002I/75A50120F33002. Infrastructure support and resources for this work were provided in part by NCATS of the NIH, grant numbers UL1TR002345, U24TR001608, U24TR001579, UL1TR001453, UL1TR003017, UL1TR003107, UL1TR002645, UL1TR001430, UL1TR001881, UL1TR002366, UL1TR003096, UL1TR002489, UL1TR001998, UL1TR002553, UL1TR002377, UL1TR002544, UL1TR002319 and UL1TR001445. Janssen provided infliximab, Bristol Myers Squibb provided abatacept, and AbbVie provided cenicriviroc for use in this trial but did not provide financial support. Gilead Sciences provided remdesivir for use in this trial but did not provide financial support.
About Washington University School of Medicine
WashU Medicine is a global leader in academic medicine, including biomedical research, patient care and educational programs with 2,800 faculty. Its National Institutes of Health (NIH) research funding portfolio is the third largest among U.S. medical schools, has grown 52% in the last six years, and, together with institutional investment, WashU Medicine commits well over $1 billion annually to basic and clinical research innovation and training. Its faculty practice is consistently within the top five in the country, with more than 1,800 faculty physicians practicing at 65 locations and who are also the medical staffs of Barnes-Jewish and St. Louis Children’s hospitals of BJC HealthCare. WashU Medicine has a storied history in MD/PhD training, recently dedicated $100 million to scholarships and curriculum renewal for its medical students, and is home to top-notch training programs in every medical subspecialty as well as physical therapy, occupational therapy, and audiology and communications sciences.